Posted February 17, 2020 in Male Gynecomastia Surgery
6 minute read
Steven P Davison, MD, DDS, FACS | Ximena Pinell, MD | Katherine Long Lijoi, MS
5 Min Read
In recent years there has been a tremendous surge in interest in contouring of the male chest. Gynecomastia, or male breast tissue, is a common medical condition that affects a third of men in their lifetime. Why the sudden interest for such a prevalent condition? Clothing patterns are to blame, the Under Armour or compression workout fashion that projects a vision of health and vitality. A trip to any mall will have the senses assaulted with images of buffed bodies with defined peck muscles sheathed in tightest fitting workout shirt or less. For the not-inconsiderable population with male breast tissue, this has driven the question of what can be done!
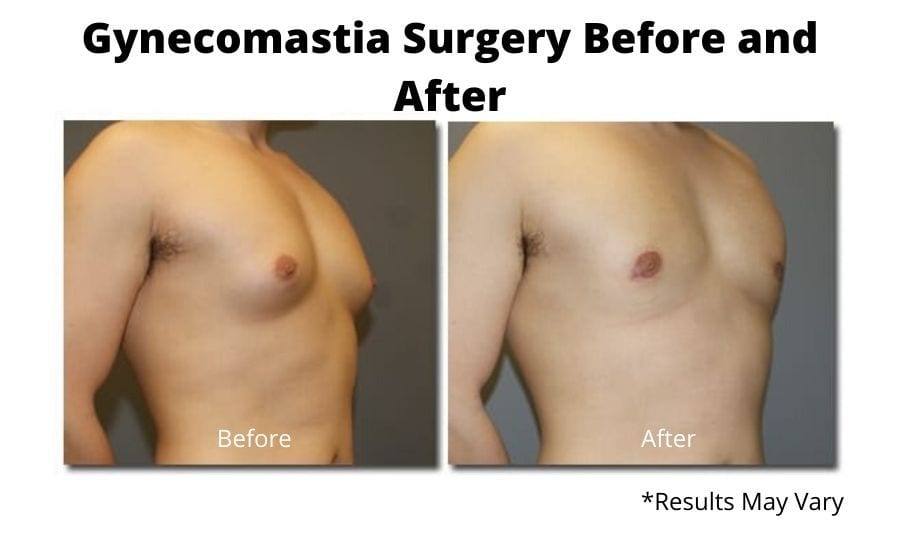
Gynecomastia, or male pattern breast tissue, is a medical condition with excess contour to the chest. It can be fat, true breast gland tissue, or a combination of both. Paradoxically, losing weight will improve a fatty male chest but will accentuate one caused by breast gland. In no way is male gland tissue a feminine trait or symptom; it is just an exaggeration of the natural breast that every man, as a mammal, has.
There are generally considered to be three causes of Gynecomastia. They can be independent or combine to make the condition more prominent. The first is a hormonal imbalance, most common in puberty. The most common time to develop gynecomastia is the worst emotional burden: while in middle school. Occasionally an endocrine or hormonal tumor can cause gynecomastia, but they are rare. The second cause is medication. Any medication that interferes with hormone balance, decreases testosterone, or increases estrogen byproducts are common culprits. Spironolactone, Propecia, Saquinavir, and cimetidine are examples of such medications. Paradoxically, some of these are medications used to reverse other psychologically traumatic conditions like male pattern hair loss. Marijuana in significant doses can cause male breast tissue to enlarge¹. The final cause is weight gain. Obesity or weight gain can cause fat to infiltrate the breast and distort the man’s chest. This is the simpler problem to address with weight loss or liposuction. Unfortunately, the stretch of the chest skin can leave a less than ideal contour.
The good news is that after a patient has been ruled out for a major medical condition by history or exam, excellent options for treatment exist. The interest in surgical solutions has taken off with Gynecomastia surgery being one of the hottest growing procedures in the field. In fact, Gynecomastia surgery increased 22.6% from 2012 to 2017². Before recommending a surgical solution, the surgeon must first determine the underlaying composition and contour of the male breast.
Size and Shape: Is the breast mostly fat or is there a pronounced presence of breast tissue located under the nipple? Is the problem of fullness alone or is there excess skin? The excess skin is much more of a problem than bulk of breast tissue. It requires contouring of the skin envelope often with additional scars. How big is the man’s areola? Is it normal sized (19-23 mm) and oval or is it bigger like a woman’s at 40+mm in size? Does it need to be reduced or reshaped into a more oval areola located lower and more to the side of the breast than that of a female patient?
Treatment Options:
Weight loss: This will only work for obesity-related, fat-infiltrated chest contour. True Gynecomastia or male pattern breast tissue will be made worse as the man’s body fat decreases. The Breast bud doesn’t reduce and with weight loss, becomes more prominent as a bump.
Liposuction: Various Liposuction techniques can contour the breast. Some deal only with fat. Other modalities such as ultrasonic accentuation (Vasar) can manage to reduce mild breast glands without open surgery.
Debridement: Mechanical debridement or rotary tools can reduce breast tissue from limited incisions. The limitation of this is completeness of the treatment and managing extra skin.
Open or Direct Surgery: This is when a limited incision around the nipple is used to remove the breast mound. Liposuction is often added to smooth out the edges.
Skin Removal: This is a more extensive treatment to address an oversized areola, drooping breast, or a severe female pattern gynecomastia, where the breast looks like a woman’s. It uses skin excision to better shape the breast to that of a man’s. The scars are usually longer but well worth the change in shape and size.
Surgery: It takes 1-2 hours based on how much is required. Unless very limited, it is more comfortable with IV sedation or general anesthesia. Most plastic surgeons use some form of tumescent fluid to reduce discomfort and decrease bleeding. The recovery is a week or so with potential for drains to collect fluid and old blood.
Scar Care: With silicone sheeting, lotions, and occasional injections scars can be softened to enhance the results. The use of a compression chest not unlike the workout shirts that started this whole conversation are common for up to a month after surgery. As the male breast is vigorously supplied with blood vessels, the risk of post-operative bleeding or hematoma is not insignificant. The very desire to have the best chest shape, that drives the request for surgery, fuels a not insignificant demand for minor revision of the chest. These should not be considered a failure, but almost an expected sequel to gynecomastia treatment.
In Conclusion: Gynecomastia, or male pattern breast tissue, is very common and nothing to be ashamed about as it affects a third of men at some time in their lives. Treatment is highly successful with excellent patient satisfaction as long as the patient and surgeon appreciate there may be tweaks to achieve the final result. It is one of the fastest growing surgical requests and most Board-Certified Plastic Surgeons will be happy to consult with you in depth on the solution that would suit you best.
Interested in Learning More?
If you would like to learn more about gynecomastia surgery in Washington, DC, contact Davinci Plastic Surgery by calling (202) 966-9590 or by filling out our online contact form.
References:
- Thompson DF, Carter JR. Drug-induced gynecomastia. Pharmacotherapy. 1993;13(1):37–45
- American Society for Aesthetic Plastic Surgery (2017). Cosmetic Surgery National Data Bank Statistics. [ebook] New York, NY: American Society for Aesthetic Plastic Surgery, p.10. Available at: https://www.surgery.org/sites/default/files/ASAPS-Stats2017.pdf [Accessed 4 Feb. 2020].